Kaiser Permanente study finds decrease reported during onset of the COVID-19 pandemic not seen in subsequent surges
The significant declines in heart attack hospitalizations and emergency care for possible strokes seen in Northern California at the beginning of the COVID-19 pandemic were not seen in subsequent surges, new research from Kaiser Permanente shows.

The study, published June 2 in JAMA, suggests public health campaigns that encouraged people to seek care if they were experiencing signs or symptoms of a stroke or heart attack were effective.
“In May 2020, we reported that, in the early months of the pandemic, the weekly number of patients admitted to our hospitals for a heart attack fell to nearly half of what would be expected,” said the study’s lead author Matthew D. Solomon, MD, PhD, a cardiologist at The Permanente Medical Group and a physician researcher at the Kaiser Permanente Division of Research. “This follow-up study suggests that we were successful in our efforts to reassure patients that it was important to leave their homes and seek emergency care if needed, and that they could do so safely.”
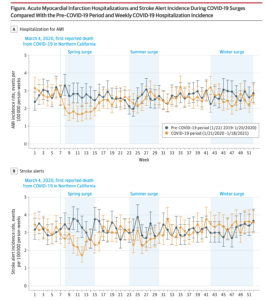
The research team analyzed weekly incidence rates for adults hospitalized with a heart attack or suspected stroke from Jan. 22, 2019, through Jan. 18, 2021 in Kaiser Permanente Northern California (KPNC), a large integrated health care delivery system. They then compared incidence rates for the time periods during the 3 COVID-19 surges in the spring (March 10 – May 4, 2020), summer (June 23 – Aug. 17, 2020), and winter (Nov. 3, 2020 to Jan. 8, 2021) to the same weeks in the prior year.
We were successful in our efforts to reassure patients that it was important to leave their homes and seek emergency care if needed, and that they could do so safely.
—Matthew Solomon, MD, PhD

The study showed weekly hospitalized heart attack and suspected stroke rates declined during the spring COVID-19 surge but then recovered to 2019 rates. During the subsequent and much larger surges in COVID-19 infections and admissions, hospitalization rates for heart attacks remained stable. A small but statistically significant decline in suspected strokes was seen during the summer COVID-19 surge, but the rates rebounded and did not decrease during the largest winter COVID-19 surge.
“In August 2020, we published research on decreased stroke presentations and discharges which made us very concerned about patients who would be at risk for long-term disabilities because they were not coming to the hospital for evaluation and treatment,” said study co-author Mai N. Nguyen-Huynh, MD, a research scientist at the Division of Research and the regional director of primary stroke for The Permanente Medical Group. “In response, we redoubled our efforts to educate our patients that if they have stroke symptoms, they should call 911 and go to the nearest stroke center. This study suggests those efforts paid off.”
 KPNC and the Division of Research were ideally positioned to carry out this research. “Our study highlights the unique ability of our embedded regional research team to respond rapidly in collaboration with a multidisciplinary team of clinical and methodological experts to gain insights from our electronic health record data to inform care planning and delivery for a large, diverse population,” said the study senior author, Alan S. Go, MD, associate director of cardiovascular and metabolic conditions research at the Division of Research and regional medical director of clinical trials for The Permanente Medical Group.
KPNC and the Division of Research were ideally positioned to carry out this research. “Our study highlights the unique ability of our embedded regional research team to respond rapidly in collaboration with a multidisciplinary team of clinical and methodological experts to gain insights from our electronic health record data to inform care planning and delivery for a large, diverse population,” said the study senior author, Alan S. Go, MD, associate director of cardiovascular and metabolic conditions research at the Division of Research and regional medical director of clinical trials for The Permanente Medical Group.

The study by Solomon and Go that showed hospitalizations fell to nearly half of what would be expected during the first months of the pandemic was published May 19, 2020, in the New England Journal of Medicine. The research by Nguyen-Huynh and her colleagues on the decrease in stroke patients reporting to the emergency room after the onset of the pandemic was published Aug. 11, 2020, in Stroke.
“Our goal is to stamp out cardiovascular disease,” said Solomon. “But until then, we want to ensure patients do not delay in seeking needed care.”
This study was supported by the Garfield Memorial Fund, and the Physician Researcher Program and the Delivery Science and Applied Research initiative of The Permanente Medical Group.
Co-authors include Thomas K. Leong, MPH and Janet Alexander, MSPH, of the Division of Research, and Jamal S. Rana, MD, PhD, and Jeffrey Klingman, MD, of TPMG.
# # #
About the Kaiser Permanente Division of Research
The Kaiser Permanente Division of Research conducts, publishes and disseminates epidemiologic and health services research to improve the health and medical care of Kaiser Permanente members and society at large. It seeks to understand the determinants of illness and well-being, and to improve the quality and cost-effectiveness of health care. Currently, DOR’s 600-plus staff is working on more than 450 epidemiological and health services research projects. For more information, visit divisionofresearch.kaiserpermanente.org or follow us @KPDOR.





Comments (0)