Kaiser Permanente study suggests blood thinners should not be routinely prescribed
COVID-19 patients who are not hospitalized are at low risk of developing blood clots and should not routinely be prescribed blood thinners, a new Kaiser Permanente research letter suggests.

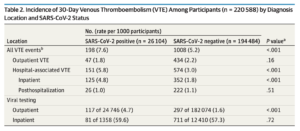
The retrospective cohort study, published in JAMA Internal Medicine, included 220,588 Kaiser Permanente Northern California (KPNC) members who were tested for COVID-19 from February 25 through August 31, 2020. In the 30 days after testing, 0.8% of the patients with a positive COVID-19 test developed a blood clot (venous thromboembolism) compared with 0.5% of the patients with a negative test result.
“Our study showed that the incidence of blood clots in outpatients who had a positive COVID-19 test and mild symptoms was similar to the incidence seen in patients who tested negative for the virus,” said the study’s senior author Ashok Pai, MD, a hematologist/oncologist with The Permanente Medical Group.

Preventing blood clots in COVID patients has been a concern since the start of the pandemic. “It was recognized within the first months of the pandemic that patients with COVID-19 were having more blood clots in the hospital and in the intensive care unit than other patients who were similarly ill,” said Nareg Roubinian, MD, an adjunct investigator at the Kaiser Permanente Northern California Division of Research and an intensive care doctor for The Permanente Medical Group. “This led us to reassess regional guidelines to prevent blood clots in hospitalized COVID-19 patients. At the same time, it was not clear what was the best treatment for outpatients with COVID.”
The new study helps answer that question. It found that in patients with COVID-19, blood clots were seen more often in those who were hospitalized than in those who were outpatients. It also confirmed findings from previous studies that found low rates of blood clots in COVID-19 patients after they left the hospital. “The incidence of blood clots in this group of patients is very low and no different than what we see in patients who are discharged from the hospital for other reasons,” said Pai.
Large blood clots can cause a heart attack, stroke, or blockage. Blood thinners are medications that help the blood flow smoothly and keep blood clots from forming or getting larger. Although they work well, they can also cause excessive bleeding. The Division of Research currently has a randomized phase 3 clinical trial underway looking at whether the drug thinner rivaroxaban (Xarelto) reduces the risk of blood clots, hospitalization, and death in outpatients with COVID-19.
 “Generally blood thinners are low risk,” said Roubinian. “But because they can cause bleeding you have to balance the benefit versus the risk, especially if you are considering using them to treat people with COVID-19 who are not very sick and may be at low risk for a blood clot. Our study suggests that we need to wait for the data from clinical trials to determine the best treatment approach and not routinely put all outpatients on blood thinners.”
“Generally blood thinners are low risk,” said Roubinian. “But because they can cause bleeding you have to balance the benefit versus the risk, especially if you are considering using them to treat people with COVID-19 who are not very sick and may be at low risk for a blood clot. Our study suggests that we need to wait for the data from clinical trials to determine the best treatment approach and not routinely put all outpatients on blood thinners.”
Funding for this study was provided by The Permanente Medical Group Delivery Science and Applied Research Program.
Co-authors include Jennifer R. Dusendang, MPH, Vincent Liu, MD, MS, and Julie A. Schmittdiel, PhD, of the Division of Research, and Dustin G. Mark, MD, and David R. Vinson, MD, of The Permanente Medical Group.
# # #
About the Kaiser Permanente Division of Research
The Kaiser Permanente Division of Research conducts, publishes and disseminates epidemiologic and health services research to improve the health and medical care of Kaiser Permanente members and society at large. It seeks to understand the determinants of illness and well-being, and to improve the quality and cost-effectiveness of health care. Currently, DOR’s 600-plus staff is working on more than 450 epidemiological and health services research projects. For more information, visit divisionofresearch.kaiserpermanente.org or follow us @KPDOR.





Comments (0)