Kaiser Permanente study teams enroll members in large, national trials setting new standards for care
Many people believe clinical trials are only for really sick people who have no other treatment options. But that’s not the case. In the cardiology field, clinical trials may test new medications to prevent or treat a wide range of diseases. That’s how the drugs called statins came to be widely used to lower cholesterol to prevent a first heart attack or stroke.
 Other research studies are designed to identify lifestyle or nutritional support approaches to improving heart health. That’s how Kaiser Permanente researchers learned that medically tailored meals may benefit recently hospitalized patients with heart failure.
Other research studies are designed to identify lifestyle or nutritional support approaches to improving heart health. That’s how Kaiser Permanente researchers learned that medically tailored meals may benefit recently hospitalized patients with heart failure.
And still others compare new surgical approaches and devices for treating structural heart problems. That’s why patients now have the option to have a transcatheter aortic valve replacement (TAVR) rather than open heart surgery.
Alan S. Go, MD, a senior research scientist at the Kaiser Permanente Division of Research, is the regional medical director for the Kaiser Permanente Northern California (KPNC) Clinical Trials Program. Interventional cardiologist Jacob M. Mishell, MD, is the medical director of the KPNC Structural Heart Program. We spoke with them about the types of cardiology clinical trials and research studies offered to KPNC members.
Why does Kaiser Permanente offer clinical trials?
Alan Go, MD: Clinical trials are really about providing enhanced clinical care as a service to our members. Yes, there is a research component, in that we randomize people to a Treatment A versus Treatment B to learn which may be more effective. But it’s really about providing access to novel treatments, elevating our care to give members the opportunity to potentially benefit from the newest treatment options, and inform the broader medical community about ways to optimize care.
What types of clinical trials are open to patients?
Go: We have cardiology prevention trials that can involve medications or lifestyle interventions. These trials fit very well within Kaiser Permanente’s overall focus on prevention. We also have cardiology treatment trials, which could include medications, procedures and devices, along with lifestyle interventions. We also conduct implementation and quality improvement trials that help us optimize care delivery within Kaiser Permanente. We are a trial site for many of the large national studies that are comparing new cardiology treatments, but we also develop and design studies that are conducted solely within KPNC.
What is structural heart research?
Jacob M. Mishell, MD: Structural heart studies have become a huge research area. This field came into existence about 12 years ago, and it focuses on fixing mechanical problems with the heart. This might be heart valves that have become too narrow or are leaky, or it may mean repairing holes in the heart.
Because the field is so young, and because it is accelerating so quickly, it means that every day we have more questions than answers. I really feel it’s important for KPNC to be involved in the studies trying to answer those questions. Patients, families, and doctors have to make treatment decisions, and the answers we get from these clinical trials give us information that helps to guide these decisions.
How do you decide what clinical trials should be offered at KPNC?
Mishell: My job is to make sure that if you are a KPNC member you have the same access to excellent health care — whether it’s standard of care or care within the context of a clinical trial protocol — that you would have if you went to another medical center. I am very passionate about that, which is why we are part of the high-profile national clinical trials answering questions in this field.
Our goal is to make sure that every patient has access to all available options for their treatment.
— Alan S. Go, MD
What do many people not know about clinical trials?
Mishell: Being in a clinical trial offers a lot of additional medical supervision in addition to potentially accessing a novel therapy. We are learning about new treatments within a structure and system that includes institutional review boards, national steering committees, and data safety monitoring teams, which is important when you are charting new territories.
How can KPNC patients learn if they qualify for a clinical trial?
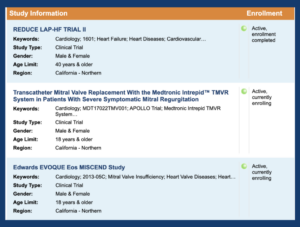
 Go: All of our active clinical trials and research studies are listed on KPStudySearch. Trials are open to patients throughout the region, but, depending on the trial and the type of treatment or procedure it involves, the patient may have to be seen at one of our cardiology subregional hubs, which are in Sacramento, San Francisco, and Santa Clara. But even if that’s the case, there may be follow-up care that can be done in their local facility, so that they don’t have to continue to travel to a specific facility.
Go: All of our active clinical trials and research studies are listed on KPStudySearch. Trials are open to patients throughout the region, but, depending on the trial and the type of treatment or procedure it involves, the patient may have to be seen at one of our cardiology subregional hubs, which are in Sacramento, San Francisco, and Santa Clara. But even if that’s the case, there may be follow-up care that can be done in their local facility, so that they don’t have to continue to travel to a specific facility.
Also, patients should know they don’t always have to look for these trials on their own. We have active TPMG physician investigators who are looking for patients who meet the criteria for the studies that we offer. Our goal is to make sure that every patient has access to all available options for their treatment.
Why should someone take part in a clinical trial?
Mishell: The most important reason is altruism. We all benefit from those who have taken part in the clinical trials that have led to the treatments we have now that are considered standard of care. Clinical trials also offer the potential for personal clinical benefits as well. I have found that there are some patients who want to be part of what’s less well known and what might have potential advantages and that there are other patients for whom uncertainty is hard enough, without adding on participating in a clinical trial. No one is obligated to take part, and if a patient decides they no longer want to participate, they just tell us — and that’s the end of the discussion. We only want people to participate if they feel it is right for them.





Comments (0)