New Kaiser Permanente study suggests working and living conditions may be key contributors to disproportionate impact of COVID-19 in communities of color
Holding a public-facing job considered “essential” and living in a multigenerational household — both of which facilitate transmission of an airborne virus — may be key contributors to the higher COVID-19 infection rates seen early in the pandemic in the U.S. in Black, Latinx, and Asian adults, a new Kaiser Permanente study suggests.

“There has been a lot of research on racial and ethnic disparities in getting tested for COVID, getting sick from COVID, and dying from COVID,” said the study’s senior author Richard Grant, MD, MPH, a research scientist at the Kaiser Permanente Division of Research. “We expected that pre-existing health problems and social risk factors would explain the differences in our population’s COVID-19 infection rates. But they didn’t. Instead, our findings suggest essential service jobs where you have to interact with the public and multiple generations living in one household were behind the disparities.”
The study published February 2 in the Journal of General Internal Medicine included 26,741 adult Kaiser Permanente Northern California (KPNC) members insured by Medicaid and 58,802 Kaiser Permanente Colorado members insured by Medicare Advantage. Every member had completed a survey within the past 2 years that included questions about social risk factors, such as food insecurity, housing concerns, and mental stress.
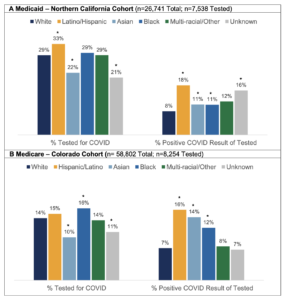
The research team reviewed members’ electronic medical records to identify those who had been tested for COVID-19 between March 1 and Nov. 30, 2020. In the KPNC cohort, 7,548 adults were tested for COVID-19; of these, 933 (12%) tested positive. In the KP Colorado group, 8,253 members were tested, and 684 (8%) were positive. Overall, 16% to 18% of Latinx, 11% to 14% of Asian, and 11% to 12% of Black members tested positive for COVID-19, compared to 7% to 8% of white members.
. . . our findings suggest essential service jobs where you have to interact with the public and multiple generations living in one household were behind the disparities.
— Richard Grant, MD, MPH
To help explain these differences, the researchers conducted statistical analyses that took into account underlying health problems, such as obesity or diabetes, and self-reported social risk factors, which disproportionally impact communities of color. But even after taking these into account, the disparities remained. The researchers said this pointed to other aspects of inequity, such as having jobs where you don’t get sick pay or time off and living in multigenerational households.
Communities of color are more likely to experience these working and living conditions. A 2018 Pew Research Study found that 1 in 5 people in the U.S. live in a multigenerational household. However, rates were higher among Asian, Black and Latinx families than white families. In addition, the Center for Economic Policy and Health Research found Asian, Black, and Latinx adults were overrepresented in frontline essential jobs, making up more than 40% of this workforce.
The researchers say the findings expand on previous studies published by the Division of Research that have identified racial and ethnic disparities in COVID-19 infection rates that could potentially influence how governments develop policies to respond to a pandemic or determine who to prioritize for vaccination.
“We may have been able to decrease transmission in communities of color if had we had prioritized vaccination of all adults who had essential jobs or who lived in a multigenerational household,” said Grant. “We might also be able to address this disparity by developing programs that make it possible for people to take paid sick leave from an essential job or isolate if they live in a multigenerational household.”
This research was supported by Kaiser Permanente’s Garfield Memorial Fund.
Co-authors include Jodi K. McCloskey, MPH, Connie S. Uratsu, RN, MS, PHN, from the Division of Research; Jennifer L. Ellis MBA, MSPH, Melanie L. Drace, MPH, and Elizabeth A. Bayliss, MD, MSPH, from the Kaiser Permanente Colorado Institute for Health Research, and James D. Ralston MD, MPH, from the Kaiser Permanente Washington Health Research Institute.
# # #
About the Kaiser Permanente Division of Research
The Kaiser Permanente Division of Research conducts, publishes and disseminates epidemiologic and health services research to improve the health and medical care of Kaiser Permanente members and society at large. It seeks to understand the determinants of illness and well-being, and to improve the quality and cost-effectiveness of health care. Currently, DOR’s 600-plus staff is working on more than 450 epidemiological and health services research projects. For more information, visit divisionofresearch.kaiserpermanente.org or follow us @KPDOR.





Comments (0)