Investigators find clues in large database of Kaiser Permanente members
People can look to the Northern European side of their genetic heritage for increased risk of nonmelanoma skin cancer, according to the first large analysis of genetic risk factors for cutaneous squamous cell carcinoma in diverse populations with European ancestry. The study was published Dec. 14 in the journal Communications Biology.

The authors examined people of varying race and ethnicity who participated in the Kaiser Permanente Research Program on Genes, Environment and Health (RPGEH). They focused on the Genetic Epidemiology Research on Adult Health and Aging (GERA) cohort, a subgroup of more than 100,000 Kaiser Permanente Northern California members who volunteered their genetic and medical information for research.
“We knew that people of European ancestry with lighter skin have a higher risk of cutaneous squamous cell carcinoma,” said lead author Hélène Choquet, PhD, a staff scientist with the Kaiser Permanente Division of Research (DOR). “We wanted to find out the risk both within and between European ancestry populations and other populations, and whether there are genetic factors involved, and it appears that there are.”
Cutaneous squamous cell carcinoma is a common cancer and its incidence is increasing not only in non-Hispanic white people but also in Latinos and Asians. While it is not usually life-threatening, if allowed to grow it can become disfiguring, spread, and even become deadly.
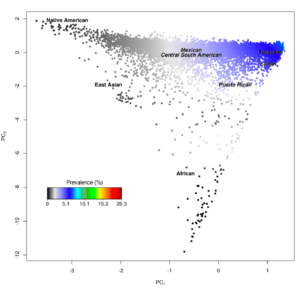
Latinos are complex to study because they may have ancestry deriving from multiple continents; a 2015 study of the GERA cohort by the same research group found most of those who described themselves as Latinos have European genetic ancestry along with Native American ancestry, and some have evidence of African ancestry as well.
In this study, the researchers examined records of 11,396 people with cutaneous squamous cell carcinoma and 86,186 control subjects in the GERA cohort and found widely varying risk by race or ethnicity group: 14% for non-Hispanic white people, compared with 3.5% for Latinos, 0.8% for East Asians, and 0.4% for African Americans.
The analysis went on to consider genetically predicted skin pigmentation, genetic risk factors for cutaneous squamous cell carcinoma, and a clinical marker for chronic sun exposure (actinic keratoses). This found that skin pigmentation accounts for a large amount of the difference within and between white people and Latinos, but not all of it. Sun exposure is also a major contributing factor.
For Latinos, the percentage of Northern European ancestry at one particular location in the genome (the SLC24A5 locus) was strongly correlated with cutaneous squamous cell carcinoma risk. The researchers also found that this risk could differ among Latinos, depending on which version of a genetic variant they inherited at the SLC24A5 locus, which is known to influence skin pigmentation.
“These findings suggest skin pigmentation alone may not be the primary determinant of cutaneous squamous cell carcinoma in Latinos, but rather the specific genetic factors underlying that pigmentation,” said co-author Neil Risch, PhD, an adjunct investigator with DOR and the founding director of the Institute for Human Genetics at the University of California, San Francisco.
“This is a striking example of a health disparity due largely to genetics,” Risch said. “The GERA cohort had limited numbers of East Asian and African American patients with cutaneous squamous cell carcinoma so we could not do a deep genetic analysis in this study but future research should explore these populations to better understand the role of their genetics and environmental exposures. For example, East Asians, who also have fair skin, appear to be strongly protected from the same skin cancer.”
Lifestyle factors such as sun exposure, use of sunscreen, and smoking also affect skin cancer risk, as does immunosuppression and use of certain medications.
“For clinicians, the research is a reminder that our patients of Latino ethnicity, particularly those with a lighter skin phenotype, are at risk for skin cancer, and would benefit from increased awareness, education, and skin cancer screening initiatives,” said senior author Maryam Asgari, MD, MPH, an adjunct investigator with DOR, associate dermatologist at Massachusetts General Hospital, and professor of dermatology and population medicine at Harvard Medical School.
The study was funded by various grants from the National Institutes of Health.
Co-authors also included co-lead author Eric Jorgensen, PhD, a former DOR research scientist; Jie Yin and Catherine Schaefer, PhD, of DOR; and Thomas J. Hoffmann, PhD, Yambazi Banda, PhD, and Mark N. Kvale, PhD, of the UCSF Institute for Human Genetics.





Comments (0)