Participants in a Kaiser Permanente trial also improved key diabetes-related health metrics
Pregnant women with overweight or obesity better controlled their weight gain and improved health behaviors when they received a series of telephone sessions with a registered dietician, a new study from Kaiser Permanente finds. They were also better able manage their hormone levels related to insulin resistance, a potential precursor to diabetes.

The Gestational Weight Gain and Optimal Wellness (GLOW) trial compared women who were coached by phone with another similar group who received usual prenatal care. The results were published May 20 in The Lancet Diabetes & Endocrinology.
Excess weight gain among pregnant women with overweight or obesity substantially increases their already elevated risk for perinatal complications such as gestational diabetes, a Cesarean delivery, or a large-for-gestational-age infant.
The findings bolster the use of telephone coaching, which could be more convenient than office visits for busy pregnant women, particularly those with small children at home, said lead author Assiamira Ferrara, MD, PhD, senior research scientist at the Kaiser Permanente Northern California Division of Research.
“For this population, sometimes the intervention requires a lot of effort, such as going to a clinic for an in-person session,” Ferrara said. “If it’s easy to participate in the intervention, the adherence may be higher, and the intervention is more likely to be effective.”
The study investigators recruited pregnant members of Kaiser Permanente Northern California over age 18 and with a body mass index between 25 and 40; they randomly assigned 200 of them to the GLOW intervention and 198 to usual prenatal care.
The GLOW intervention involved 2 in-person sessions and 11 telephone sessions on behavioral strategies to manage weight and improve diet and physical activity. Its design was adapted from the national Diabetes Prevention Program behavioral intervention that was shown to reduce the risk of type 2 diabetes by 58% in high-risk women. Usual care during the trial period (2014 to 2017) involved medical visits and periodic health education newsletters.
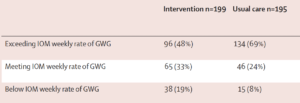
The proportion of women exceeding the Institute of Medicine guidelines for gestational weight gain was significantly lower in the intervention group being coached by phone (48%) than in the usual care group (69%). Women who were coached gained an average of 10.21 kg (22.5 lbs) while those in usual care gained an average of 12.36 kg (27.2 lbs). The coached women also had lower caloric intake, especially from saturated fat, and less sedentary behaviors than those who had usual care.
Blood levels of key biomarkers related to diabetes were also better in the GLOW group; these included insulin, leptin, and homeostatic model assessment, an index of insulin resistance.

“The results from this rigorous trial are very strong,” said coauthor and Division of Research biostatistician Charles Quesenberry, PhD. “However, the trial did not have the statistical power to assess group differences in perinatal complications. Larger trials are needed to assess whether reducing gestational weight gain also reduces perinatal complications.”
The GLOW intervention focused on assisting women to change their health behaviors by “meeting them where they are” rather than being prescriptive, said coauthor Monique Hedderson, PhD, a research scientist with the Division of Research. “The intervention was delivered using motivational interviewing techniques, trying to get women to think about what’s possible for them. The coaching helped women set small realistic goals that were achievable and strategize to problem-solve in ways that were specific to them.”
GLOW was built on previous trials from the same research team, including the Gestational Diabetes Effects on Moms (GEM) trial, showing that telemedicine was effective in reducing gestational weight gain, postpartum weight retention, and the proportion of neonates that were large for their gestational age. Results of GEM were published in Diabetes Care in 2016 and 2018.
The research team is carrying out follow-on work testing a mobile phone app as a method to coach at-risk pregnant women with overweight and obesity to avoid excess weight gain.
Providing women with ongoing guidance on lifestyle changes towards healthy weight creates tremendous benefits to both the patient and the health care system. “By having regular, personal, and more convenient follow-up, a woman is more likely to be successful and feel supported while needing fewer office visits.”
–Kari Carlson, MD, director of regional women’s health Kaiser Permanente Northern California and The Permanente Medical Group
The GLOW trial was funded by a grant from the Eunice Kennedy Shriver National Institute of Child Health and Human Development.
Coauthors included Charles P. Quesenberry, PhD, Ai-Lin Tsai, MS, Juanran Feng, MS, and Maren Galarce, MPH, of the Division of Research; Susan D. Brown, PhD and Samantha F. Ehrlich, PhD, adjunct investigators with the Division of Research; Santica Marcovina, PhD, of the University of Washington; and Patrick Catalano, MD, of the Mother Infant Research Institute at Tufts Medical Center.
# # #
About the Kaiser Permanente Division of Research
The Kaiser Permanente Division of Research conducts, publishes and disseminates epidemiologic and health services research to improve the health and medical care of Kaiser Permanente members and society at large. It seeks to understand the determinants of illness and well-being, and to improve the quality and cost-effectiveness of health care. Currently, DOR’s 600-plus staff is working on more than 450 epidemiological and health services research projects. For more information, visit divisionofresearch.kaiserpermanente.org or follow us @KPDOR.





Comments (0)