Kaiser Permanente research examines clinicians’ search patterns and practices
Modern medical care relies heavily on computers to track and deliver patient care, but that doesn’t mean these electronic health record (EHR) systems are widely beloved. In fact, a growing body of research indicates frustration with time-consuming computer work is one reason some physicians are unhappy in their jobs.


That’s why Kaiser Permanente Division of Research investigators decided to analyze more than 12 million search activities by users of Kaiser Permanente Northern California’s EHR – KP HealthConnect (KPHC). They theorized that understanding what users were searching for could identify potential opportunities to improve EHR use.
Their study, published March 6 in JAMA Network Open, identified top search terms for various health care professionals and analyzed the relationships among search terms. They then used these data to identify what users were looking for most – and consider how they might find it more easily.
Lead author Halley Ruppel, PhD, RN, and senior author Vincent Liu, MD, MS, both investigators with the Division of Research, discuss the results.
Q: Is the use of the search field an indication the EHR design has problems?
Ruppel: No. Similar to using the internet today, using Google search doesn’t mean the internet has failed. Instead, the search function has an important place because there is a massive amount of data in each patient’s chart. Our KPHC team deployed the search function to help our clinicians find what they need as quickly as possible. We know that some clinicians use the search field to navigate the chart efficiently. We conducted this exploratory analysis of search terms to take a data-driven approach to finding opportunities for improving EHR use.
Q: What did you find?
Ruppel: Overall, the most common search terms were statin, colonoscopy, and “PFT,” which stands for pulmonary function test. These weren’t surprising given how often these are part of the integrated health care Kaiser Permanente delivers.
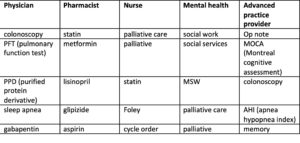
Liu: We also found that different EHR users often exhibit very different search patterns. Overwhelmingly, pharmacists searched for medications and the clinical information needed to assess medication changes. Different physician specialists also searched for very different items. For example, search patterns in adult and family medicine differed from those in neurology. This suggests there could be opportunities to further customize the EHR interface by practitioner type. Past research has shown that EHR users have greater satisfaction with their experience when the interface is customized for them.
Ruppel: Among mental health practitioners, top search terms included social work, social services, and LCSW (licensed clinical social worker). Serial searches for similar concepts could mean that clinicians were having difficulty locating notes and information related to these services in the chart. This is an example of how these data could be used to redesign an interface to make this information easier to find.
Q: Your paper includes a complex, colorful graph of search terms. What does it mean?
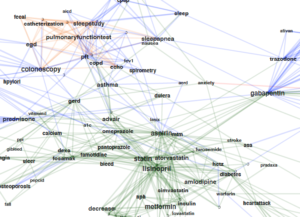
Ruppel: We created the network graph to illustrate what terms were frequently searched together in the same session in a patient’s chart. In the graph we see clusters of terms representing different domains (such as medications, imaging, and labs), focused on a particular clinical topic. One possible interpretation is that information normally grouped by domain instead of by a specific clinical topic could be better grouped within the EHR.
Q: What follow-on research are you planning on this topic?
Liu: We’re working with our KPHC team to see how these data can improve the use of the EHR to improve patient care and clinician satisfaction. Before we can make more specific recommendations, we need to work with these expert teams to contextualize these findings. Interviewing and observing clinicians to understand why they searched for certain terms will be key.
However, these findings highlight a tremendous opportunity to use these complex data to make everyday improvements that improve our care.





Comments (1)
Anything to make the physician’s desktop medicine practice easier is a real contribution. Search term analysis points the way to where opportunities lie. Great work, Halley and Vinnie. I’ll stay tuned.