Kaiser Permanente study underscores importance of managing gestational diabetes soon after diagnosis
Women with gestational diabetes who achieve blood sugar levels within the target range soon after diagnosis and maintain healthy levels through delivery are less likely to have a child with obesity than those whose blood sugar remains higher, according to new Kaiser Permanente research published in Diabetes Care.
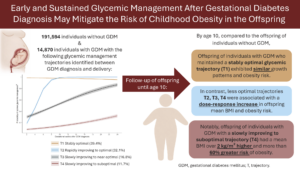
The study authors reached this conclusion after examining 206,464 Kaiser Permanente Northern California pregnancies, which included 14,870 pregnancies complicated by gestational diabetes. The pregnant patients were stratified into 4 trajectory groups based on their blood sugar levels from diagnosis through delivery. They were compared with a group of pregnant women who did not have gestational diabetes.

Children of mothers in the trajectory group that achieved blood glucose levels within the target range soon after diagnosis were less likely to develop obesity up to age 10. In fact, the rate of childhood obesity in this group was similar to that observed in women without gestational diabetes. By contrast, children of mothers in the 3 other trajectory groups faced a higher risk of childhood obesity.
The results provide patients and their care teams with valuable insights for managing this pregnancy complication, said lead author Rana Chehab, PhD, MPH, RD, a staff scientist with the Kaiser Permanente Division of Research.
“Our goal with this study is to send a hopeful message: pregnant patients with gestational diabetes who are empowered and supported to address their blood sugar levels promptly after diagnosis can improve their child’s long-term health,” Chehab said. “When healthy glucose levels are achieved soon after diagnosis, it may help reduce the risk of obesity later in childhood.”
 One in 5 American children has obesity, and increasingly this is starting at very young ages with long-lasting health consequences. “Once a child develops obesity, it becomes much more difficult to return to a healthy weight,” Chehab said. “That’s why we’re looking earlier in the life course, focusing on pregnancy as a potential window to reduce a child’s future risk.”
One in 5 American children has obesity, and increasingly this is starting at very young ages with long-lasting health consequences. “Once a child develops obesity, it becomes much more difficult to return to a healthy weight,” Chehab said. “That’s why we’re looking earlier in the life course, focusing on pregnancy as a potential window to reduce a child’s future risk.”
Gestational diabetes during pregnancy is one of the major risk factors for childhood obesity. Other contributors include children’s diets, screen time, physical activity, and social factors such as the food environment they encounter at home, school, or daycare.
Previous research looking at whether treatment of gestational diabetes lowers the risk of childhood obesity has largely reported no clear effect, Chehab said. But the current analysis was unique in the ability to track glucose levels throughout the pregnancy rather than relying on 1 or 2 glucose readings from a pregnancy. It also followed children for up to 10 years and beyond through their routine well-check visits with pediatricians, allowing researchers to assess longer-term outcomes.
Unique KPNC support program
All patients with gestational diabetes were enrolled in the Kaiser Permanente Regional Perinatal Service Center program, a structured telehealth-based care model that provides regular glucose monitoring, treatment adjustments (including medications when needed), and counseling on diet and physical activity.

Within the program, patients fell into 4 glycemic management trajectory groups over the course of their pregnancies: stably optimal (39.4%), rapidly improving to optimal (32.1%), slowly improving to near optimal (16.8%), and slowly improving to suboptimal (11.7%).
“Kaiser Permanente Northern California’s standardized, centralized perinatal management program is a strong model for coordinating prompt, intensive support for patients newly diagnosed with gestational diabetes,” said co-author Mara Greenberg, MD, a maternal-fetal medicine specialist with The Permanente Medical Group who directs the Regional Perinatal Service Center. “The program is run by registered nurses and registered dietitians who stay in close contact with patients to monitor their progress and support healthy glucose levels. It has been highly effective, with the majority of women in the program falling into the 2 most optimal trajectory groups.”
The analysis took into account the mother’s pre-pregnancy overweight or obesity diagnosis and severity of gestational diabetes when they were diagnosed, and found those factors did not change the results.

The study team published an earlier analysis in 2022 in JAMA Network Open with DOR Research Scientist Yeyi Zhu, PhD, serving as senior author, that looked at the role of these same glucose control trajectories in pregnancy on complications at birth including cesarean delivery, large-for-gestational-age baby, dislocation of the baby’s shoulder during delivery, or admission to the neonatal intensive care unit. That study found lower rates of poor pregnancy outcomes with early and consistent glucose control.
“This new analysis builds on our prior work by showing that the benefits of early and sustained glycemic management, starting as soon as gestational diabetes is diagnosed, not only help protect mothers and infants from complications at birth, but may also have longer-term benefits in reducing the risk of childhood obesity,” said Zhu, a co-senior author of the Diabetes Care study.

“What’s really powerful about this work is that it reflects the collaboration between the Division of Research and our medical centers, where findings from studies can directly inform evidence-based care,” said co-senior author Assiamira Ferarra, MD, PhD, a DOR research scientist who leads the Center for Upstream Prevention of Adiposity and Diabetes Mellitus. “There is the need to identify barriers and facilitators for achieving glycemic control to help patients to manage their blood glucose levels and we are doing this investigation in another study that will inform potential actional targets for patients with gestational diabetes.”
The study was funded by the National Institute of Child Health and Human Development, the National Institute of Diabetes and Digestive and Kidney Diseases, and Kaiser Permanente Community Health.
Additional co-authors were Amanda L. Ngo, MPH, and Juanran Feng, MS, of the Division of Research, and Catherine Lee, PhD, formerly of the Division of Research.
###
About the Kaiser Permanente Division of Research
The Kaiser Permanente Division of Research conducts, publishes, and disseminates epidemiologic and health services research to improve the health and medical care of Kaiser Permanente members and society at large. KPDOR seeks to understand the determinants of illness and well-being and to improve the quality and cost-effectiveness of health care. Currently, DOR’s 720-plus staff, including 73 research and staff scientists, are working on nearly 630 epidemiological and health services research projects. For more information, visit divisionofresearch.kp.org.





Comments (0)