Large Kaiser Permanente study finds risk is higher in breast cancer survivors than in women who have not had breast cancer
Breast cancer survivors are at greater risk of developing high blood pressure and diabetes than women who have never been treated for breast cancer, new Kaiser Permanente research shows.

“We suspected that cardiometabolic health problems might be common among breast cancer survivors,” said the study’s lead author Marilyn L. Kwan, PhD, a senior research scientist at the Kaiser Permanente Division of Research. “Our study is one of the largest to date to focus on the specific cardiometabolic problems these women are at risk for and the specific cancer treatments that may increase their risk.”
The study, published January 13 in the Journal of Clinical Oncology, compared risk for high blood pressure, diabetes, and abnormal cholesterol levels over an average 7 years of follow-up in 14,942 women diagnosed with breast cancer enrolled in the Kaiser Permanente Northern California (KPNC) Pathways Heart Study and 74,702 female KPNC members without breast cancer who were of a similar age, race, and ethnicity.
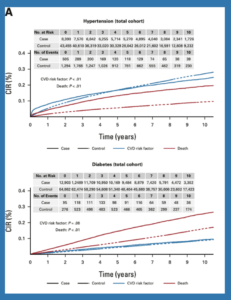
The study showed a cumulative high blood pressure incidence rate of 10.9% in the breast cancer survivors and 8.9% in the women without breast cancer 2 years after cancer diagnosis. For diabetes, there was a cumulative incidence rate of 9.3% among the breast cancer survivors compared to 8.8% among the women without breast cancer up to 10 years later.

“Diabetes and hypertension are 2 of the biggest risk factors for heart disease,” said study co-author Jamal S. Rana, MD, PhD, an adjunct investigator with the Division of Research and a cardiologist with The Permanente Medical Group. “Our findings of additional confluence of these risk factors point to the need for even more vigilance and preventive care to mitigate risk in breast cancer survivors.”
The diabetes risk was higher in women whose breast cancer treatments included chemotherapy, left-sided radiation therapy, or endocrine therapy; the risk for high blood pressure was higher in women who had left-sided radiation or endocrine therapy. Women who were normal weight at the time of their diagnosis were also at higher risk of developing diabetes and high blood pressure than those who had overweight or obesity.
“Prior to conducting this study, we knew that many breast cancer treatments are cardiotoxic, but we did not have a good understanding of the magnitude of these effects on increasing risk for cardiometabolic abnormalities in women who have been treated for breast cancer,” said senior author Heather Greenlee, ND, PhD, MPH, associate professor at Fred Hutchinson Cancer Research Center. “These study results quantify the increased risk and show us the impact on women’s long-term health.”
Our study is one of the largest to date to focus on the specific cardiometabolic problems these women are at risk for and the specific cancer treatments that may increase their risk.”
— Marilyn L. Kwan, PhD
Over the past decade, oncologists and cardiologists have begun to work more closely together to meet the needs of cancer patients who have received treatments that have the potential to cause heart damage. This new study builds on and contributes to that effort.
 “There is growing recognition of overlap in the underlying mechanisms and risk factors that occur concurrently with cancer and cardiovascular disease,” said study co-author Richard Cheng, MD, MSc, director of the University of Washington Cardio-Oncology Program.
“There is growing recognition of overlap in the underlying mechanisms and risk factors that occur concurrently with cancer and cardiovascular disease,” said study co-author Richard Cheng, MD, MSc, director of the University of Washington Cardio-Oncology Program.
The researchers say the findings highlight the importance of talking to patients about their long-term risk for diabetes and high blood pressure and what they can do to reduce that risk.
“Sometimes patients put other health conditions to the side and focus on their breast cancer,” said study co-author Dawn Hershman, MD, MS, the director of the Breast Oncology Program at Columbia University Medical Center. “It is important for them to know that they are at risk for these other health problems, that their risk may be higher either from the treatment or the physical consequences of being diagnosed, and that they should do as much as they can to prevent weight gain, exercise, stay adherent to all of their medications and follow up with their other health care providers.”
Kwan said she and her colleagues would now like to conduct research that can help determine the best ways to evaluate and address cardiometabolic risk factors in breast cancer survivors. “Identifying this risk is the first step in improving health outcomes in our breast cancer patients,” she said. “Now, we want to look more closely at the best interventions that health systems can make to reduce this risk.”
The study was funded by the National Cancer Institute.
Co-authors include Carlos Iribarren, MD, MPH, PhD, Romain Neugebauer, PhD, Mai Nguyen-Huynh, MD, MAS, Lawrence H. Kushi, ScD, Cecile A. Laurent, MS, Valerie Lee, MHS, and Janise M. Roh, MSW, MPH, of the Division of Research; Zaixing Shi, PhD, Hanje Shen, MS, Eileen Rillamus-Sun, PhD, MPH, and Margarita Santiago-Torres, PhD, of the Fred Hutchinson Cancer Research Center.
# # #
About the Kaiser Permanente Division of Research
The Kaiser Permanente Division of Research conducts, publishes and disseminates epidemiologic and health services research to improve the health and medical care of Kaiser Permanente members and society at large. It seeks to understand the determinants of illness and well-being, and to improve the quality and cost-effectiveness of health care. Currently, DOR’s 600-plus staff is working on more than 450 epidemiological and health services research projects. For more information, visit divisionofresearch.kaiserpermanente.org or follow us @KPDOR.





Comments (0)